Materials & Chemicals

Click Chemistry-Based Multi-Enhanced Biomaterials Help Heal Wounds
WARF: P100330US02
Inventors: Weiyuan John Kao, Yao Fu
The Wisconsin Alumni Research Foundation (WARF) is seeking commercial partners interested in developing advanced, biomaterial-enabled, cell-based wound healing therapies.
Overview
Wound healing is a complex and dynamic process of rebuilding skin and tissue. Chronic or impaired wounds result when tissues fail to progress through the necessary stages of healing. This is a significant clinical problem, affecting 5.7 million patients in the United States and costing an estimated $20 billion each year.
The choice of treatment and the development of novel therapeutics depend on the underlying biology and co-morbidity. Although current understanding of many cellular and molecular processes has advanced substantially, efficacy of single agent therapeutics is disappointing and more than 50 percent of wounds remain refractory to conventional treatment.
In addition, current cell-based epidermal and/or dermal equivalents are costly and laborious to manufacture. Some are not applicable to the care of acute wounds or indicated for full-thickness defects. Furthermore, all epidermal/dermal equivalents are used only temporarily to provide factors released from the cells to the wound bed.
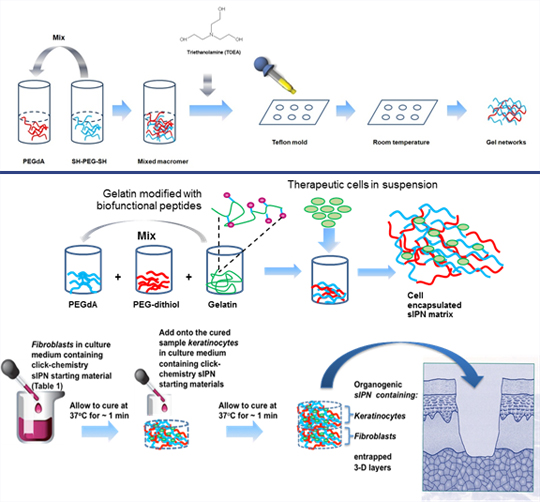
UW–Madison researchers previously developed improved wound dressing materials that use biofunctionalized biomaterials to recapitulate tissue structure lost due to trauma or underlying disease to improve healing (see WARF reference number P01328US). These materials include semi-interpenetrating networks (sIPNs), a platform material that mimics the extracellular matrix and presents factors like therapeutic cells that promote healing to the wound bed. The sIPNs use a multi-functional hydrogel as a scaffold for damaged tissues. The polymer material consists of a biochemically-modified and cross-linked gelatin matrix, onto which are grafted various heterodifunctional polyethylene glycols (hPEGs). The hPEGs increase the biocompatibility and durability of the hydrogel and also provide attachment sites for therapeutic molecules. The biodegradable matrix allows for temporally and spatially controlled delivery of bioactive signals to modulate and complement the dynamics of the wound healing process, making these materials functional and clinically viable as wound dressings.
The choice of treatment and the development of novel therapeutics depend on the underlying biology and co-morbidity. Although current understanding of many cellular and molecular processes has advanced substantially, efficacy of single agent therapeutics is disappointing and more than 50 percent of wounds remain refractory to conventional treatment.
In addition, current cell-based epidermal and/or dermal equivalents are costly and laborious to manufacture. Some are not applicable to the care of acute wounds or indicated for full-thickness defects. Furthermore, all epidermal/dermal equivalents are used only temporarily to provide factors released from the cells to the wound bed.
UW–Madison researchers previously developed improved wound dressing materials that use biofunctionalized biomaterials to recapitulate tissue structure lost due to trauma or underlying disease to improve healing (see WARF reference number P01328US). These materials include semi-interpenetrating networks (sIPNs), a platform material that mimics the extracellular matrix and presents factors like therapeutic cells that promote healing to the wound bed. The sIPNs use a multi-functional hydrogel as a scaffold for damaged tissues. The polymer material consists of a biochemically-modified and cross-linked gelatin matrix, onto which are grafted various heterodifunctional polyethylene glycols (hPEGs). The hPEGs increase the biocompatibility and durability of the hydrogel and also provide attachment sites for therapeutic molecules. The biodegradable matrix allows for temporally and spatially controlled delivery of bioactive signals to modulate and complement the dynamics of the wound healing process, making these materials functional and clinically viable as wound dressings.
The Invention
The UW–Madison researchers have now adapted “click chemistry” in lieu of an external energy source to form the sIPNs. This allows a wider variety of sensitive bioactive molecules, including therapeutic cells, to be entrapped within the sIPNs, enhancing the clinical applicability of the technology.
Applications
- Wound healing
- Primary wound dressing
- Surgical and dental wound packing material
Key Benefits
- Eliminates need for external energy sources to induce polymerization, which allows more molecules and live cells to be incorporated into sIPNs and enhances the clinical applicability of the technology
- Allows production of greater variety of sIPNs
- Chemistry is easy to perform.
- Material is biocompatible, biodegradable, safe and effective.
- Adheres to tissue and conforms to complex contours to facilitate delivery of active biomolecules
- Maintains moist healing environment and provides barrier to pathogens
- Functionalizable to promote healing and address co-morbidity
- Cost-effective to synthesize and manufacture with long shelf life
- Easily adaptable to current clinical practice
- Compatible with most current advanced wound therapies
- Easy patient compliance with minimal bandage changes
- Facile, in situ cell entrapment without the labor intensive procedure for current epidermal/dermal equivalence
Tech Fields
For current licensing status, please contact Jeanine Burmania at [javascript protected email address] or 608-960-9846
Figures